People shouldn’t put off having regular screenings for breast and colon cancer.
By: Michelle Martin, for St. Joseph Hospital
Health screenings have significantly decreased since the start of the pandemic – but the need for them is more important than ever. Even young adults shouldn’t skip regular screenings. After all, doctors are increasingly discovering cancer among all age groups – often in people with no family history.
Screenings for cancer and other diseases can detect issues early when they are most treatable. Cancer screenings allow doctors to detect precancerous lesions in their beginning stages, often before symptoms appear.
Some people, especially those in their 20s, 30s and 40s, have delayed or canceled health screenings due to COVID-19, but it is very safe – and very necessary – to have them done. And by finding an experienced medical team near you, critical screenings are accessible and can be conveniently scheduled.
“Cancer doesn’t wait for COVID, and neither should you,” said Dr. Prasanna Gulur, a gastroenterologist at St. Joseph Hospital.
The importance of regular screenings
Dr. Gulur likens screenings to an old saying.
“An ounce of prevention is worth a pound of cure,” he said. “This rings especially true for colorectal cancer. Colon cancer is very common; it is preventable. And should you have it, the earlier it is found, the greater the chances for survival.”
Stage 1 colon cancer has a survival rate of 80-95%. At stage 2, the survival rate drops between 55 and 80%. When colon cancer is in stage 3, it falls to 40%. By stage 4, there is only a 10% chance of a cure.
Likewise, breast cancer screenings can find cancer early – and they can save lives.
“Since regular mammography screening began in the United States in the 1980s, the breast cancer death rate has decreased by over 35%,” said Dr. Kira Wendorf, medical director of the Breast Care Center at St. Joseph Hospital. “Early detection with mammography not only saves lives, but also reduces the severity of treatment that women with breast cancer must undergo. Studies have demonstrated that women whose breast cancers are found with screening mammography are less likely to have more intensive treatment, such as mastectomy or chemotherapy.”
In addition to colonoscopies and mammograms, other important screenings include those to detect cervical and HPV, skin and prostate cancers.
Regular screening is important in young adulthood – and beyond. Beginning at age 21, women should have pap smears for cervical cancers. In general, men and women should begin being screened for skin cancer in their 20s – or sooner if they have a family history of skin cancer or spend a lot of time in the sun. Men should also begin being screened for prostate cancer earlier than age 50, if they have a family history of the disease.
Two important health screenings can be completed right at St. Joseph in Nashua, including colorectal and breast cancer screenings.
Colorectal screenings
Colonoscopies are a common way to screen for colon cancer, but there are other screenings as well. They include stool-based screenings, X-rays, CT-based radiological tests and a limited endoscopic exam called a flexible sigmoidoscopy.
“All of the GI societies consistently endorse that the best option is the one that gets done,” Dr. Gulur said. “Whatever option you choose is better than not getting screened.”
People with no personal or family history of colon polyps or colon cancer should have their first screening at age 45. Those with a family history or genetic predisposition should start sooner.
“We have multiple excellent screening options and they have been shown to save lives by study after study,” he said. “All the options are 100% covered by health insurance providers as their benefits are universally accepted.”
Dr, Gulur said one of the most misunderstood things that he hears from patients is that they skip screenings because they don’t have a family history of colon cancer, or they don’t have symptoms.
“It’s all about education: 90% of patients diagnosed with colon cancer have no family history,” he said. “And colon cancer produces symptoms only at late stages where the chances of survival are significantly lower than if caught by screening.”
Patients should talk with their doctor if they have any concerns about screenings.
“If you’re still undecided, have a frank discussion with your primary care provider and find the best option that works for you,” he said.
Breast cancer screenings
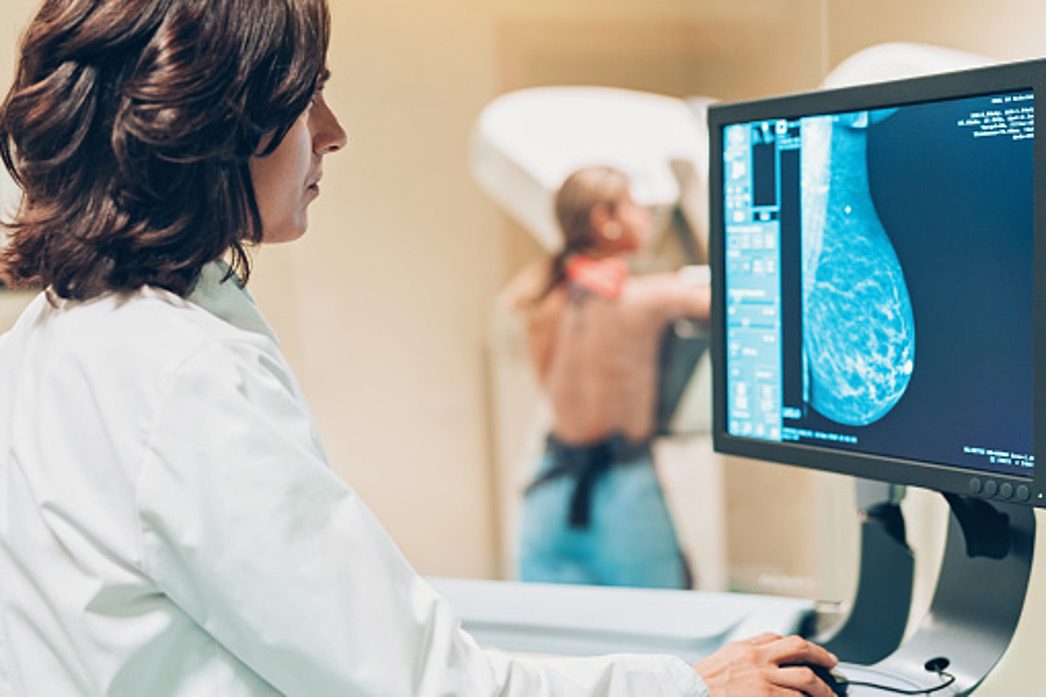
St. Joseph Hospital recommends that women begin having a yearly mammogram beginning at age 40. For women who have an elevated lifetime risk of developing breast cancer, additional screening modalities – such as screening ultrasounds and breast MRIs – might also be recommended.
“One in six breast cancers occur in women between the ages of 40-49 years old,” Dr. Wendorf said. “By not getting a yearly mammogram after age 40, women increase their odds of dying from breast cancer, and that treatment for any advanced cancers ultimately found will be more extensive and more expensive.”
St. Joseph Hospital offers 3D mammography, also known as digital breast tomosynthesis (DBT), a new technique that is more accurate than standard mammography. Other screenings include breast ultrasounds, breast MRIs and stereotactic, ultrasound and MRI-guided breast biopsies.
“We screen each patient on their individual lifetime risk of developing breast cancer and offer supplemental screenings to those who qualify,” she said. “We can identify patients who may meet criteria for and benefit from genetic counseling/testing and have a APRN who offers genetic testing should they be interested.”
Like Dr. Gulur, Dr. Wendorf also has seen a number of patients delay a screening due to COVID-19. She urges patients not to delay. The Breast Care Center at St. Joseph Hospital follows expert guidelines from the American College of Radiology and the Centers for Disease Control and Prevention (CDC) to safely conduct non-emergency care, such as mammograms and screenings.
There is only one reason to delay having a mammogram – and that’s only to delay for several weeks. Because the COVID-19 vaccine causes some women to develop swollen lymph nodes under their arm on the same side as their injection, Dr. Wendorf recommends scheduling a mammogram before having the first vaccine or waiting four weeks until after the second one.
But no matter what, she urges patients to schedule a mammogram even if they don’t have a family history of cancer.
“Approximately 75% of women diagnosed are the first person in their family to be diagnosed,” she said, “and do not have any identifiable risk factors.”
The hometown team at St. Joseph agrees this underscores the critical importance of staying up to date with regular screenings, contributing to a stronger community that’s healthier – at every age.